Researchers Develop Way to Measure Blood Pressure Using a Camera and AI
![]()
Engineers from the University of South Australia and Baghdad’s Middle Technical University have designed a way to measure blood pressure with no physical contact using a camera and artificial intelligence (AI).
The researchers believe that the method can replace existing methods for measuring systolic and diastolic pressure that use a “cumbersome” strap and inflatable cuff wrapped around a patient’s arm or wrist.
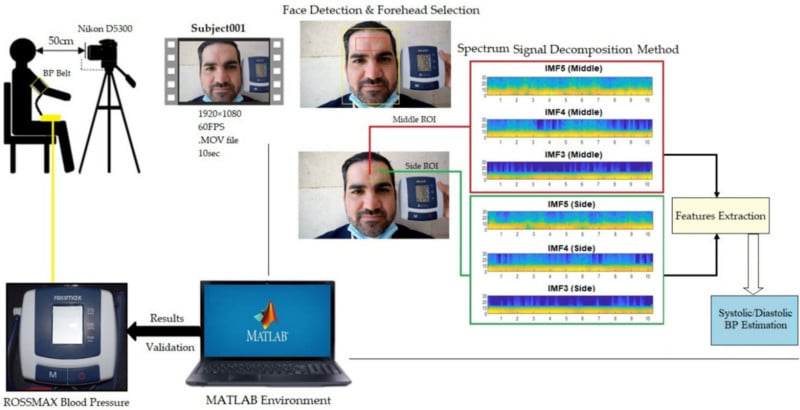
The new technique, which has been published in a full research paper, involves filming a person from a “short distance” for 10 seconds with a consumer-grade camera (specifically, a Nikon D5300 is mentioned in the research paper) and extracting cardiac signals from two regions of the forehead using AI algorithms.
This method was derived from a demonstration first shown in 2017 when a University of South Australia and Iraqi research team were able to extract a human’s heart rate from a drone video. Since then, researchers have been able to develop mutliple algorithms to measure vital signs at a distance, including breathing rates from a distance of up to 50 meters, oxygen saturation, and temperature.
“Monitoring blood pressure is essential to detect and manage cardiovascular diseases, the leading cause of global mortality, responsible for almost 18 million deaths in 2019,” UniSA remote sensing engineer Professor Javaan Chahl says in a report from the University of South Australia.
“Furthermore, in the past 30 years, the number of adults with hypertension has risen from 650 million to 1.28 billion worldwide. The health sector needs a system that can accurately measure blood pressure and assess cardiovascular risks when physical contact with patients is unsafe or difficult, such as during the recent COVID outbreak. If we can perfect this technique, it will help manage one of the most serious health challenges facing the world today.”
To test the system, the team tried the method on 25 different people of varying skin tones and in a variety of lighting conditions, which were challenges introduced in order to overcome limitations with this technique noted in previous studies.
According to the engineers, the experiments resulted in systolic and diastolic readings that were about 90% accurate. The team says that these results are very good, especially considering that the existing strap-based instrument is not always accurate and is “subject to errors.”
Image credits: Header photo via the University of South Australia Public Relations.